Follow us on Google News (click on ☆)
These results, published in Nature Immunology, open up new perspectives for developing preventive strategies against respiratory allergies.

Illustration image Pixabay
The steady increase in respiratory allergies and asthma in industrialized countries raises a puzzle: why do some individuals develop allergies while others do not? One hypothesis suggests that "exposure to microbes" prevents this phenomenon. But the mechanism remained unknown.
Researchers from the Pasteur Institute and Inserm led by Gérard Eberl, head of the Microenvironment and Immunity unit, and Lucie Peduto, head of the Stroma, Inflammation and Tissue Repair unit, wanted to test this hypothesis directly. Their discovery is remarkable: exposure of the lung to microbial fragments induces long-lasting immune memory that effectively blocks subsequent allergic reactions, and this lasts for several months.
The key experiment: long-lasting protection
The scientists exposed the lungs of mice to fragments of viruses or bacteria, which triggers a type 1 immune response — the one the body naturally deploys against these microbes. When these mice were simultaneously exposed to an allergen, they were completely protected for at least six weeks.
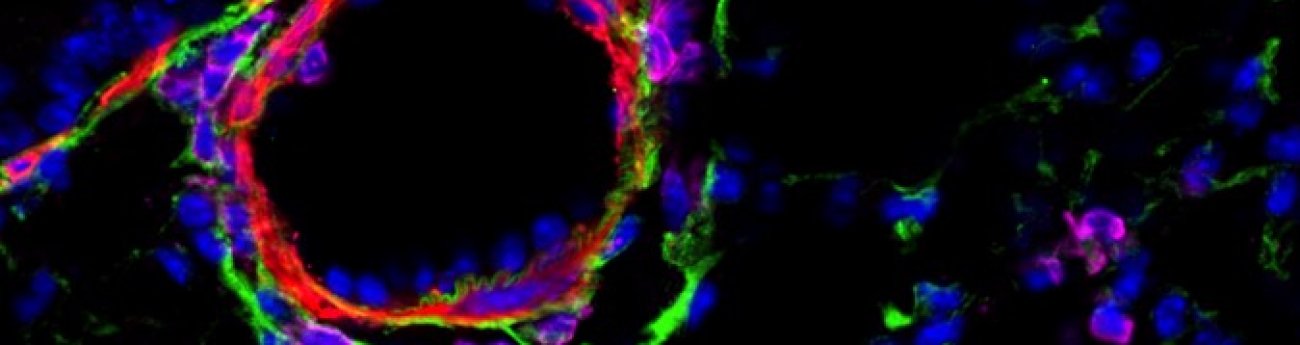
How microbes protect against allergyStromal cells (in green) that carry the memory, around a bronchiole (smooth muscle in red), and immune cells (in pink) recruited for the occasion.
© Institut Pasteur
Another discovery: pre-exposure of mice to microbial fragments protected them durably for more than 3 months against subsequent reactions. In the absence of this initial protection, the mice developed a massive reaction characterized by an accumulation of a type of immune cell (eosinophils) in the lungs.
Without this protection by microbial fragments, a first exposure to the allergen "programmed" the lungs toward hypersensitivity, and then upon re-exposure, the allergic reaction intensified catastrophically.
Fibroblasts, unexpected players in immune memory
Where was this protective memory stored? Although classic immune cells — B and T lymphocytes — have long been considered the main actors in immune memory, a detailed analysis of lung cells revealed the key role of fibroblasts.
Fibroblasts are almost "ordinary" cells: they form the structure of the lung, participate in wound healing, support and direct immune cells. What is special about them? An epigenetic modification of the Ccl11 gene which codes for the CCL11 molecule, or eotaxin, responsible for recruiting eosinophils, the masters of the allergic reaction.
"In mice, we observed that when the lung triggers a type 1 immune response, induced by viruses or bacteria, it durably blocks the Ccl11 gene in fibroblasts. This epigenetic modification persists for months and completely protects the lungs against allergic reactions. It is truly a tissue memory that persists long after the disappearance of the immune cells present during the initial infection," explains Amy Blondeau, co-first author of the study, a researcher within the Microenvironment and Immunity unit at the Pasteur Institute.
Implications for allergy prevention
This discovery opens several clinical perspectives.
On one hand, it justifies prophylactic interventions. The early administration of agents stimulating a type 1 immune response (like OM-85, already used in the clinic) could durably prevent the development of allergies. This would be a real prevention strategy, and not just symptomatic treatment.
On the other hand, the study encourages targeting fibroblasts instead of focusing solely on the immune system. Future therapies could directly correct the epigenetic programming of fibroblasts to protect against allergens.
The team continues to explore ways to translate this fundamental discovery into therapeutic approaches. To do this, they will work on answering the remaining questions. In children, how long could an infection protect against allergies? How can interventions be optimized to induce this protection? Can this protective memory be restored in people who are already allergic?